|
8/14/2023 0 Comments Kayexalate potassium antidote 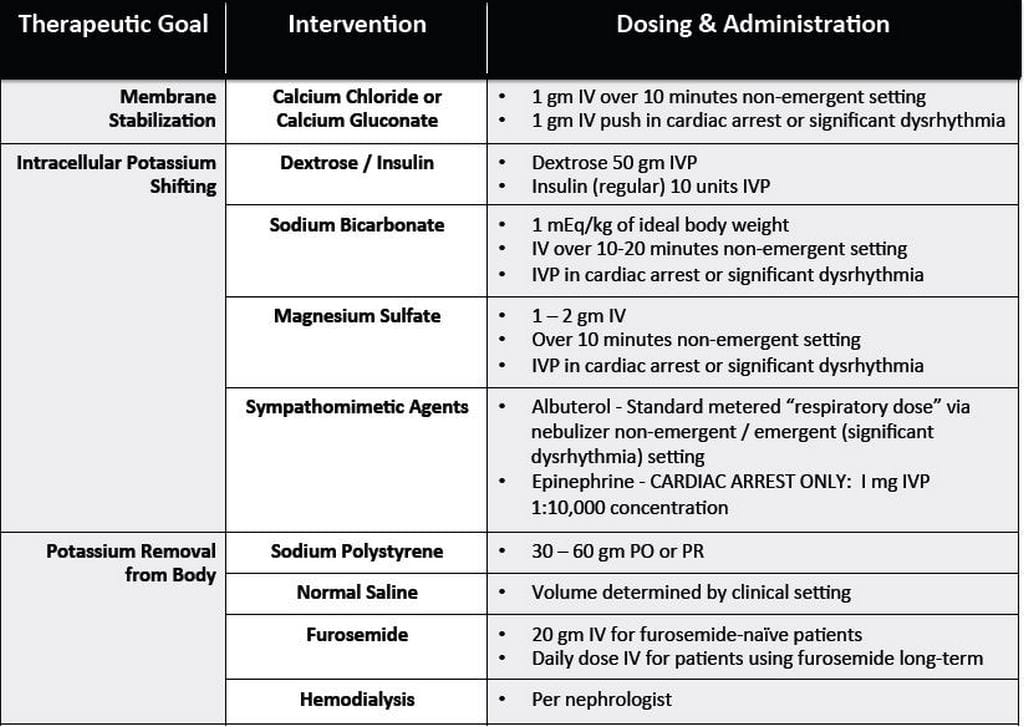
ECG signs of toxicity include prolongation of the QT interval. Cocaine is the most common street drug that increases the incidence of pulseless arrest. Street drugs and other chemicals can precipitate pulseless arrest. Some of the most common include tricyclics, digoxin, beta-blockers, and calcium channel blockers. Core temperature should be raised above 86 F (30 C) as soon as possible.Īccidental overdose of a number of different kinds of medications can cause pulseless arrest. The hypothermic patient may be unresponsive to drug therapy and electrical therapy (defibrillation or pacing). If a patient has been exposed to the cold, warming measures should be taken. Hypoglycemia was removed from the H’s but is still to be considered important during the assessment of any person in cardiac arrest. Treat hypoglycemia with IV dextrose to reverse a low blood glucose. Hypoglycemia or low serum blood glucose can have many negative effects on the body, and it can be associated with cardiac arrest. Never give undiluted intravenous potassium. Always follow the appropriate infusion standards. Treatment of hypokalemia involves rapid but controlled infusion of potassium. The major signs of hypokalemia or low serum potassium are flattened T-waves, prominent U-waves, and possibly a widened QRS complex. Read more about hyperkalemia with cardiac arrest here. All of these will help reduce serum potassium levels. 
This can be treated in a number of ways which include sodium bicarbonate (IV), glucose+insulin, calcium chloride (IV), Kayexalate, dialysis, and possibly albuterol. Also, a widening of the QRS-wave may be seen. The major sign of hyperkalemia or high serum potassium is taller and peaked T-waves. Hyper-/hypokalemiaīoth a high potassium level and a low potassium level can contribute to cardiac arrest. Prevent metabolic acidosis by giving the patient sodium bicarbonate. Prevent respiratory acidosis by providing adequate ventilation. To determine if the patient is in respiratory acidosis, an arterial blood gas evaluation must be performed. Also, ensure that your oxygen source is connected properly. You must ensure that the patient’s airway is open and that the patient has chest rise and fall and bilateral breath sounds with ventilation. Hypoxia or deprivation of adequate oxygen supply can be a significant contributing cause of cardiac arrest. A fluid challenge or fluid bolus may also help determine if the arrest is related to hypovolemia. After CPR, the most important intervention is obtaining intravenous access/IO access. Looking for obvious blood loss in the patient with pulseless arrest is the first step in determining if the arrest is related to hypovolemia. Hypovolemia or the loss of fluid volume in the circulatory system can be a major contributing cause of cardiac arrest. Toxins, Tamponade(cardiac), Tension pneumothorax, Thrombosis (coronary and pulmonary), and Trauma. Hypovolemia, Hypoxia, Hydrogen ion (acidosis), Hyper-/hypokalemia, Hypoglycemia, Hypothermia. These H’s and T’s will most commonly be associated with PEA, but they will help direct your search for underlying causes to any of arrhythmias associated with ACLS. The H’s and T’s of ACLS is a mnemonic used to help recall the major contributing factors to pulseless arrest including PEA, Asystole, Ventricular Fibrillation, and Ventricular Tachycardia. Knowing the H’s and T’s of ACLS will help prepare you for any ACLS scenario. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
